
The term ‘nRBC’ refers to precursor cells of the red blood cell lineage which still contain a nucleus; they are also known as erythroblasts. nRBC content correlates with CD 34+ cells and, in fact there is a positive correlation between higher nRBC content and engraftment. “nRBC count is used for the measurement of speed of engraftment”. “High nRBC counts identified CBUs that engrafted faster than units supplying the same Total count (TC) dose but lacking nRBCs”. An average nRBC contribute 8% of CB nucleated cells, with a wide range noted after normal term delivery (range 0% – 42%). With conventional plasma depletion / red cell depletion techniques used in cord blood banking, a large proportion of nRBCs remain within the CB product and thus contribute to the final TNC (range 0% – 36%) There was a concern that high nRBC content in the TNC would have a misleadingly high estimation of hematopoietic potential of a cord blood unit. (1, 2)
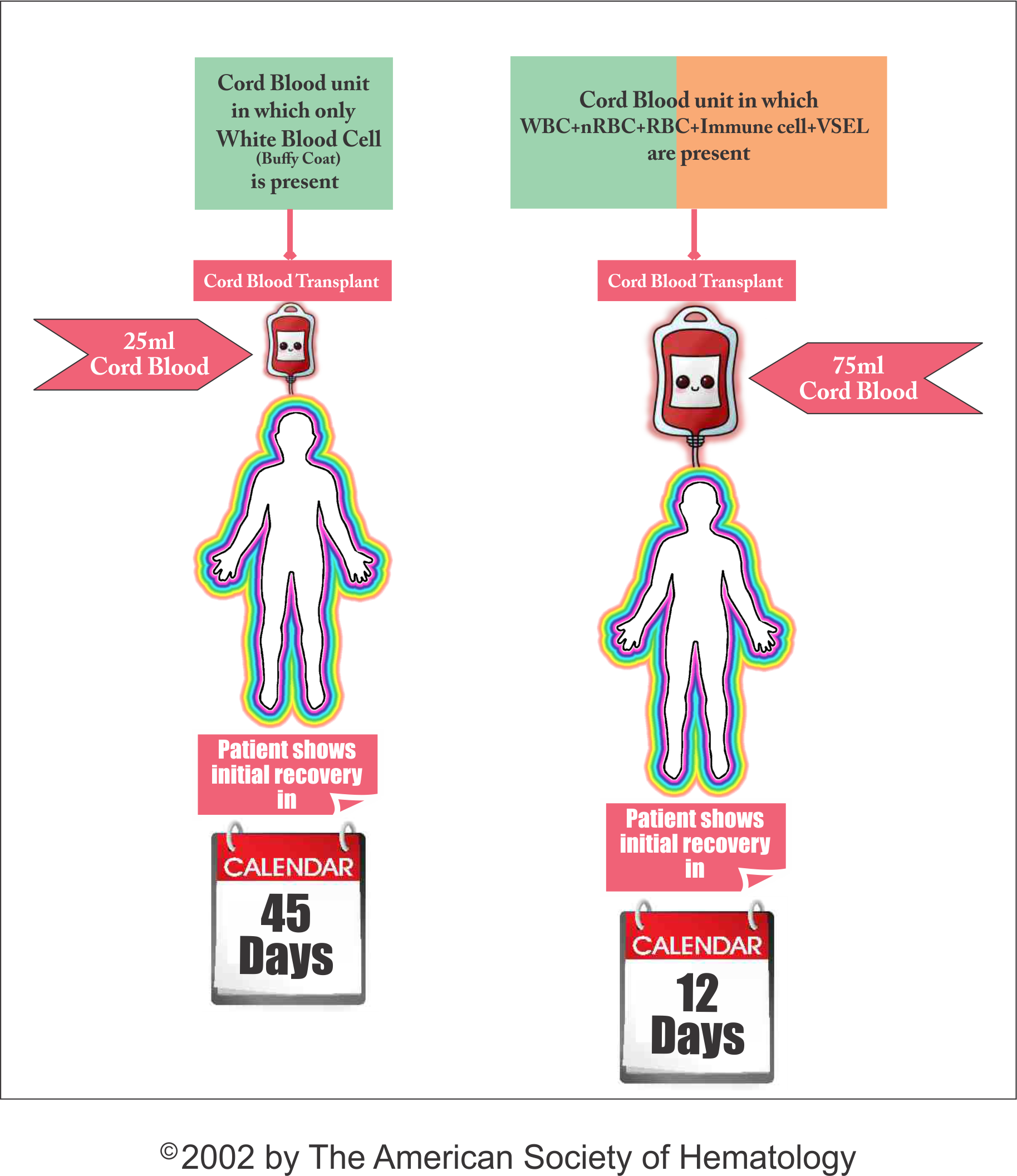
Few studies explored the possible influence on engraftment of nucleated red blood cells (nRBCs) in the graft. nRBCs were counted by visual examination or by using an automated analyzer. nRBCs correlated with progenitor cell numbers. Both white blood cell and nRBC dose were independently predictive of myeloid engraftment speed. Because nRBC dose predicted engraftment speed, inclusion of nRBCs in the TNC count does not reduce the effectiveness of the prefreezing TNC count as an index of the quality of a Placental Cord Blood (PCB) unit as a graft. The correlation between the number of nRBCs and the number of hematopoetic progenitor cells probability reflects the involvement of early stem cells in erythroid responses.
References :
- UK Government website release. Available athttps://www.- gov.uk/drug-device-alerts/drug-alert-hydroxyethyl-starch-hes-products- increased-risk-of-renal-dysfunction-and-mortality (accessed February 2015).
- https://books.google.co.in/books?id=vp8X5R4YzQsC&pg=PA339&lpg=PA339&dq=nrbc+in+cord+blood+transplant&source=bl&ots=k0FyTcM09w&sig=4mv_3unwteToD6BFJNm80Vap2A4&hl=en&sa=X&ved=0ahUKEwjlxTC7_LQAhUHRI8KHfnpALoQ6AEIRTAI#v=onepage&q=nrbc%20in%20cord%20blood%20transplant&f=false

